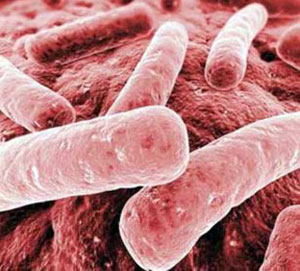
 The Centers for Disease Control and Prevention (CDC) recently released a warning about a particular strain of bacteria that is wreaking havoc in hospitals across the U.S. It is called Carbapenem-Resistant Enterobacteriaceae, or CRE for short. The name of the bacteria comes from the family of antibiotics called carbapenems. They are drugs of last resort when other antibiotics do not work on an infection. Unfortunately, these bacteria are now showing resistance to carbapenems. The CDC is concerned because that means this strain of bacteria is now resistant to nearly all antibiotics currently available.
The Centers for Disease Control and Prevention (CDC) recently released a warning about a particular strain of bacteria that is wreaking havoc in hospitals across the U.S. It is called Carbapenem-Resistant Enterobacteriaceae, or CRE for short. The name of the bacteria comes from the family of antibiotics called carbapenems. They are drugs of last resort when other antibiotics do not work on an infection. Unfortunately, these bacteria are now showing resistance to carbapenems. The CDC is concerned because that means this strain of bacteria is now resistant to nearly all antibiotics currently available.
Bacteria like the CREs are often called superbugs because they are so difficult to kill. The result is that people are dying from bacterial infection, something that seemed unthinkable just a couple of decades ago. So far, infections with CRE are still fairly rare and are only being seen in hospitals and nursing homes, but they are killing people. Doctors are resorting to using an antibiotic called polymixin because nothing else will stem the infection. Unfortunately, the reason this drug is not widely used is because it also causes kidney failure. The choice for some patients becomes death by bacteria or renal failure.
Bacteria
Bacteria are one of the earth’s oldest and simplest life forms. They are single-celled organisms, and they outnumber all other organisms on the planet. In fact, your body contains more bacterial cells than your own. We would not survive without these little life forms, but some of them cause infection, diseases, and even death.
Bacteria reproduce through a process called binary fission. Each cell grows to a certain size, copies its genetic material, and then splits in two. They do this quickly. A colony of bacterial cells can double in a matter of minutes. This quick reproduction means that bacteria can evolve quickly as well. This is the key to antibiotic resistance.
Antibiotics
Also known as antimicrobial drugs, antibiotics are medications that fight bacterial infections by killing bacterial cells. The first antibiotic, penicillin, was discovered in 1928 by Alexander Fleming. This led to the development of more drugs that could be used to kill bacteria. The first medical use of antibiotics occurred in the 1940s and it revolutionized medicine. Before antibiotics, death from bacterial infection was common. Today, we forget how different life was before antibiotics could cure simple illnesses like strep throat or an ear infection.
Learn How To Make Your Own Emergency Remedies For Use In Any Survival Situation …
Different antibiotics work in different ways, but they all kill bacterial cells. Drugs are classified by the way in which they operate and destroy cells. Penicillins, for instance, act on the cell wall or membrane and disrupt it. Quinolones and sulfonamides interfere with enzymes in bacterial cells. Tetracyclines act on the synthesis of proteins. Some antibiotics are narrow-spectrum, meaning they target one or two species of bacteria, while others are broad-spectrum and kill a range of bacteria.
Overuse Of Antibiotics
The current problem that the CDC has recognized is not new. Before CRE, the concern was VRE bacteria, and before that MRSA, or resistant staph bacteria. The reason that these bacteria become resistant to antibiotics is because they divide and reproduce quickly and evolve quickly. Bacteria can evolve to develop resistance to drugs. They are a tough life form, and this ability to evolve into so many different forms is why they have been around on the earth since it first began.
We have spurred this evolution of antibiotic resistance by overusing the medications that are no longer working on some bacteria. Every time bacterial cells are exposed to antibiotics and survive, they have the opportunity to evolve resistance. They can change their enzymes, their proteins, or their cell walls in order to overcome the drug. The more we use antibiotics, the more opportunities the bacteria have to evolve and change.
This ability to quickly evolve in the face of an antibiotic is why the drugs come with a warning to finish the course of antibiotics. If you have ever taken antibiotics, your doctor warned you to keep taking the full course, even if you start to feel better. Taking the full course ensures that you kill every one of the infecting bacteria. If you do not kill them all, the ones that survive can evolve to develop resistance to that drug, and your infection will come back, stronger than ever. When we overuse antibiotics, we do this on a worldwide scale and create superbugs that cannot be killed with any antibiotic we have.
What To Do?
The solution to the problem is to limit the use of antibiotics to situations in which they are truly needed. For example, many people confuse bacteria with viruses. Viruses are different from bacteria. They are smaller and even simpler than bacteria. Unlike bacteria, they cannot live long outside the body of an animal. Viruses cause illness and disease, but they cannot be killed by antibiotics. Too often, people see their doctor when they are sick and are prescribed antibiotics when really, the infection is viral. The common cold, for instance, is viral, not bacterial. Doctors prescribe antibiotics anyway because it makes patients feel better to have some sort of “treatment.” The practice needs to stop.
Another overuse of antibiotics is the prevalence of antibacterial soaps. Washing your hands thoroughly with warm water and regular soap is enough to adequately remove bacteria. The use of antibiotics in soaps is unnecessary and has only contributed to the evolution of antibiotic-resistant strains. Factory farming is another source of overuse of antibiotics. Farm animals are pumped full of antibiotics to prevent disease. According to the FDA, factory farms use 30 million pounds of antibiotics every year. Those antibiotics end up in the food and water supply.
Everyone can do their part to slow the evolution of bacteria into antibiotic-resistant superbugs. Stop using antibacterial soaps, only use a course of antibiotics when it is necessary, and stop supporting factory farms. It is also important to prevent infections when you have a wound. You can use hydrogen peroxide, soap and water, or rubbing alcohol. If a wound becomes infected in spite of your best efforts, however, you may need antibiotics. It is important to remember that you should use antibiotics when they are needed. If your doctor says you need a course to fight a particular illness, you need to do so. If everyone uses antibiotics wisely and only when necessary, we can stop these superbugs from forming.
 Off The Grid News Better Ideas For Off The Grid Living
Off The Grid News Better Ideas For Off The Grid Living




